Claim Denial Management With Hansei Solutions
Hansei Solutions offers claim denial management to help non-hospital and behavioral healthcare practices identify denial trends, reduce rejections, and streamline the claim and record submission process.


Claim Denial Management In Behavioral Health Billing
Claim denial management is a key component of behavioral health billing and revenue cycle management. Most patients use their health insurance plans to pay for healthcare, and it’s up to the medical practice to bill and submit a claim to the insurance or payor. Once the insurance company covers the cost of the medical services and the patient has paid any required copays or coinsurance, the healthcare practice moves on to the next patient, and the cycle begins again.
As healthcare becomes more complicated and insurance companies expand their plans to cover more services, their guidelines and regulations can overwhelm small or untrained providers with denied claims. Multiple unresolved denied claims can drain behavioral healthcare providers’ revenue and impact every part of their practice, including staff, doctors, equipment, and patient care.
The most recent reports estimate that each claim resubmittal can cost providers more than $100 per claim, not including the initial cost of submitting the claims, the possibility of further denials after reworking, and the impact on cash flow. Another study revealed that two-thirds of denied claims can be recovered, but 65% are never worked on again, costing providers thousands of dollars in potential unclaimed revenue. When factoring in the cost of denials and follow-ups, medical practices can begin to lose revenue quickly

Identifying Claim Denial Reasons
As a revenue cycle management and behavioral health billing company, we at Hansei constantly analyze our experiences to continue making advancements and educate ourselves on the best solutions. Claim denials can originate from the clinical side of care due to a procedure denied as medically necessary or because it was performed by an out-of-network physician and the administrative office, ranging from coding errors to improperly submitted claims. Other common causes of denials include:
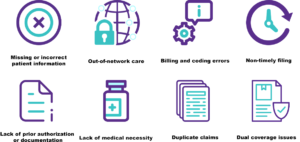
Addressing Root Causes
Some of the biggest challenges faced by behavioral healthcare providers today include:
Insufficient Training
30% to 40% of denied claims stem from challenges related to registration and pre-service procedures. In physician practices, particularly smaller ones, staff members often face a heavy workload and juggle various administrative tasks while keeping up with the ever-changing industry and regulatory requirements.

Lack of Automation
One-third of healthcare providers still rely on manual processes for claim denial management. Such manual approaches are prone to human error, offer limited transparency, consume significant time, and lead to delays in processing claims.

Lack of Resources
Denied claims can seem insignificant at first, but some practices struggle to recover enough revenue to cover the costs of correcting and appealing denied claims. Similarly, without a dedicated team to effectively prioritize, manage, and route claims, providers find it challenging to handle their denial management processes and receive reimbursement from payors.
Our Claim Denial Management Services Include

Audit Management
Our audit management services offer a practical way to control behavioral healthcare expenses. These services include validating diagnosis-related groups (DRG), handling clinical appeals, conducting retrospective audits, and assisting with under-billed audits.

Effective Denial Management
As part of our revenue cycle management approach, we focus on effectively handling denials to control costs. Our goal is to reduce the number of denied claims while improving overall strategies. Our process is designed to be hassle-free and doesn’t require constant supervision from your behavioral healthcare staff.

Expertise and Technology
Our years of experience and multifaceted backgrounds in healthcare and medical billing, combined with one of the most advanced EHR systems, help you address pain points, like common denial reasons, and simplify internal workflows. You’ll have real-time access to the status of denials and can contact our experienced team for questions or suggestions.

Managing Appeals Process
If an appeal is necessary after resubmitting a claim, we’ll efficiently manage the process until its final adjudication. Our denial management team constantly seeks opportunities to enhance our approach. If we discover better strategies for addressing denials or improving claim submissions, we collaborate and strategize to implement those improvements.
Hansei’s Claim Denial Management Process
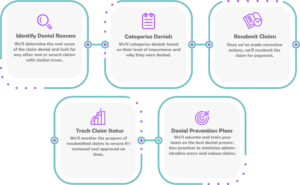
Benefits of Claim Denial Management
More Clean Claims: Our denial management process focuses on identifying the root causes of denials and implementing preventive measures. We’ll help you improve your clean claims rate and reduce administrative burdens and costs.
Boosted Net Revenue: Our denial management strategies ensure that you receive the maximum reimbursement for your services. By minimizing denials and addressing issues promptly, you can capture revenue that may have otherwise been lost.
Better Patient Care & Loyalty: Denied claims can frustrate patients and create a negative experience if their healthcare is paused during the appeal process. By efficiently managing denials and reducing payment delays, you can provide a smoother billing process for happier patients.
Improved Operations & Lower Costs: Our denial management services help optimize your operations by streamlining claim submission processes and reducing rework costs. By preventing denials and focusing on clean claims, Hansei can save your practice hundreds of hours of valuable staff time and resources.
Direct Lines To Growth: Hansei Solutions’ dedicated team stays informed about the latest coding guidelines, payer requirements, and denial prevention strategies, ensuring that your practice remains compliant and efficient in managing claim denials.

Ready to focus on providing healthcare? Let us lighten your load.
We’re here to address your pain points and create growth opportunities for your organization. We’re passionate about what we do, and it shows in every interaction. Learn what makes us tick and schedule a demo today.