Blog

Table of Contents
Utilization review management is of paramount importance in the healthcare sector to guarantee that patients get necessary and suitable medical attention while curbing expenses. Utilization review evaluates the necessity and efficiency of medical treatments, procedures, and services with the help of rules and standards, which not only enhances the quality of care for patients but also helps to restrain healthcare costs and manage the utilization of resources.
Continue reading to learn more about utilization review, utilization review management, the various processes involved, and the benefits of implementing utilization management programs in healthcare businesses.
What is Utilization Review?
Utilization review is the practice of assessing the necessity, suitability, and effectiveness of medical treatments, operations, and services to ensure that people get the necessary and proper care. This is usually done by health organizations, insurers, or government organizations, utilizing set guidelines and criteria. Utilization review may involve pre-approval, concurrent review, or retrospective review. The goal of utilization review is to strengthen the quality of care for patients, manage medical bills, and guarantee the right use of resources.
Why is Utilization Review Management Important?
Utilization review management is an important process that healthcare organizations must understand and properly implement. Through regular review of utilization data and implementation of best practices, healthcare organizations can optimize their operational efficiency and ensure optimal care for patients. Therefore, utilization review management is essential to ensuring the successful functioning of any healthcare organization.
Other reasons why utilization management is important include:

Quality of Care
Utilization review is an important part of the patient healthcare process that helps ensure that quality of care is provided to patients. This quality of care can be achieved by reviewing medical records to determine if the necessary and appropriate care is being given to the patient. By having this process in place, it can lead to better health outcomes for the patient, as well as increased cost savings for the organization.
Compliance
Utilization review helps healthcare organizations and providers ensure compliance with legal and regulatory requirements. This includes reimbursement rules, fraud prevention, and any other guidelines that must be adhered to. Compliance is a vital part of any healthcare organization and utilization review can help healthcare providers maintain this standard set by the relevant governing bodies.
Resource Management
Proper resource management is essential to providing quality healthcare services. Utilization review plays an important role in this, as it helps to make sure that resources are only used when necessary and used in the most effective way possible. This can reduce unnecessary costs, ensuring that healthcare resources are used appropriately and efficiently, and ultimately lead to improved patient outcomes as well as a better overall delivery of care.
Cost Control
Utilization review is an effective tool for cost control in the healthcare industry. It helps to identify and address any unnecessary or inefficient treatments, procedures, or services that are driving up costs. By implementing utilization review strategies, healthcare providers can help ensure that resources are being used responsibly and efficiently, in order to keep costs at a minimum. Utilization review is an important part of managing healthcare costs, as it helps to reduce inefficiencies that lead to increased costs.
Data Analysis
Utilization review is an effective method of data collection and analysis that can help healthcare professionals identify gaps in the system. By examining trends and patterns over time, valuable insights can be gained about where improvements can be made. This data is invaluable for creating a more efficient and effective healthcare system that better serves the needs of patients.
What are the Three Components of the Utilization Review Process?
Utilization review has three components: pre-service review, concurrent review, and retrospective review.
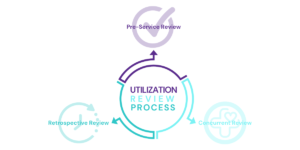
Pre-Service Review
Before healthcare services are delivered, the pre-service review is conducted to check if the proposed services are necessary and covered by the patient’s insurance. A healthcare provider submits a request for authorization of a proposed healthcare service, such as surgery or diagnostic test. The insurance company or utilization review organization reviews the request to determine if the service is medically necessary and covered by the patient’s insurance plan.
Concurrent Review
Concurrent review is done while the patient is receiving care to make sure the services are still right and necessary. During the course of care, the insurance company or utilization review organization may conduct ongoing monitoring to ensure that the services being provided are still medically necessary and appropriate.
Retrospective Review
After the patient has received care, the insurance company or utilization review organization reviews the services provided to determine if they were medically necessary and appropriate and identify any opportunities for improvement or cost savings.
Utilization Management vs. Utilization Review
Utilization management and utilization review are two distinct yet related terms in the healthcare sector. Utilization management is the practice of regulating and overseeing the utilization of healthcare resources, which includes assessing and accepting healthcare services. By contrast, utilization review is the process of examining and assessing the necessity, appropriateness, and cost-effectiveness of healthcare services before, during, and after they are dispensed to patients.
Utilization review is an element of utilization management that looks into healthcare services. Utilization management comprises a broad scope of tasks like recognizing high-cost or high-risk patients, planning for care coordination, and offering care management programs to help patients with chronic diseases. On the flip side, utilization review basically concentrates on examining healthcare services for clinical necessity and suitability and making decisions regarding coverage.
Another major distinction between utilization management and utilization review is that the former is usually carried out by health insurers to oversee medical expenses and ensure patients get the right care. Utilization review can be done by medical insurers, providers, health systems, or other groups to make sure the services rendered are medically necessary and suitable.
Benefits of Implementing a Utilization Management Program
Healthcare organizations should implement utilization review management plans as a means of controlling medical expenses while making sure that patients get the appropriate and necessary treatments. This utilization review process, which encompasses pre-service, concurrent, and post-reviews, can find and reduce redundant services, leading to cost savings for the healthcare payer and the patient. Utilization management can also make sure health professionals comply with state and federal regulations and the terms of the patient’s insurance. By introducing a utilization management program, healthcare organizations can benefit from data and analytics, since the process produces data on healthcare utilization and costs, which can be used to detect patterns and chances for progress.
Taking advantage of utilization management can better the dialogue between healthcare providers, patients, and payers, making sure that everyone is in the loop and striving for a collective objective. Additionally, utilization management can assure that patients receive suitable care that involves coordination and is applicable to their medical condition, which can decrease the chances of mistakes and problems. Last but not least, utilization management can make the healthcare system more transparent by furnishing patients and payers with data relating to the expense and quality of care. All these advantages make utilization management an indispensable instrument for healthcare organizations to manage healthcare costs and enhance patient care.
Utilization Review with Hansei Solutions
When you trust Hansei Solutions for your utilization review management needs, you’re guaranteed to receive and also provide the most accurate medical review service.
Hansei’s Utilization Review team takes pride in their personal understanding of how each facility operates, attending facility treatment team meetings with an open-communication format, allowing everyone to feel more comfortable with the role they play.
Hansei Solutions offers accredited healthcare utilization management services that can be modified to the requirements of any healthcare provider or payer. Our services allow for better collaboration within the healthcare system and help direct members to the necessary care provided in the appropriate setting. Contact Hansei Solutions today to learn more and to get started.


Download Our FREE eBook

Ready to focus on providing healthcare? Let us lighten your load.
We’re here to address your pain points and create growth opportunities for your organization. We’re passionate about what we do, and it shows in every interaction. Learn what makes us tick and schedule a demo today.